The Hasson Trocar is an important surgical instrument used in laparoscopic and minimally invasive procedures. It is specially designed for the open laparoscopic entry technique, also known as the Hasson technique. This method provides surgeons with a safer and more controlled abdominal entry compared to blind insertion methods.
Modern laparoscopic surgeries require precision, safety, and reliable access systems. Therefore, the Hasson Trocar has become a preferred choice for surgeons performing procedures in gynecology, urology, general surgery, bariatric surgery, and colorectal surgery.
Because patient safety is the highest priority during abdominal access, surgeons widely use the Hasson Trocar to reduce the risk of injury to internal organs and blood vessels during trocar insertion.
What is a Hasson Trocar?
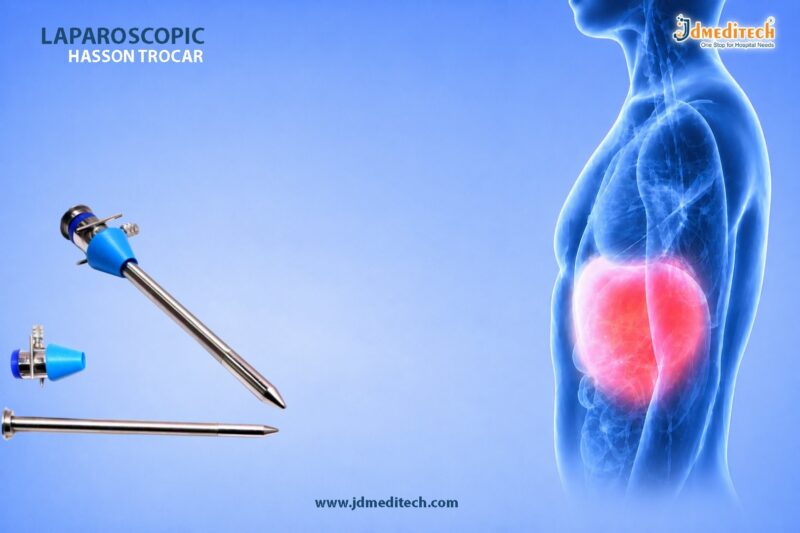
A Hasson Trocar is a blunt-tip laparoscopic trocar designed for open-entry abdominal access. Unlike sharp trocars used in closed techniques, this trocar is inserted after making a small incision under direct vision.
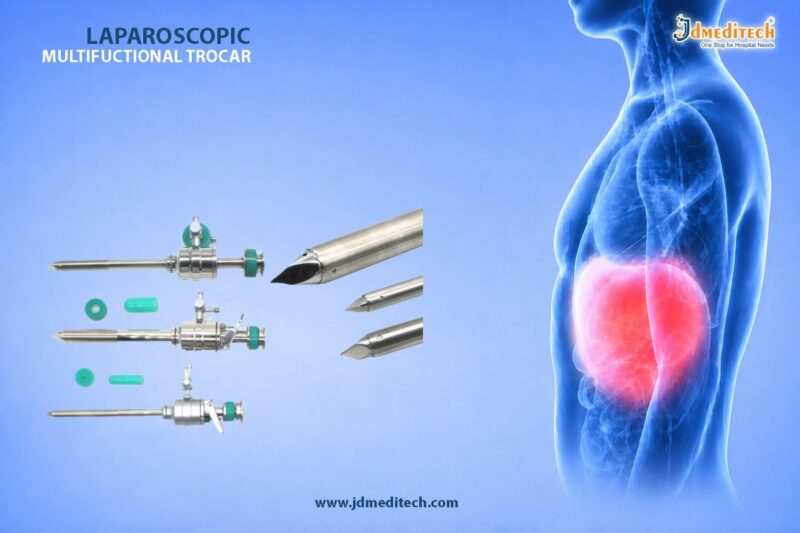
The trocar usually includes:
- Blunt obturator
- Cannula with fixation cone
- Adjustable sleeve
- Suture fixation system
- Gas sealing valve
These components help maintain pneumoperitoneum while ensuring stable and secure positioning during surgery.
Importance of the Hasson Technique in Laparoscopy
The Hasson technique was developed to improve patient safety during laparoscopic entry. In this method, the surgeon creates a small incision and directly visualizes tissue layers before inserting the trocar.
As a result, the chances of accidental injury to:
- Bowel
- Blood vessels
- Abdominal organs
are significantly reduced.
Additionally, this technique is especially beneficial in patients with:
- Previous abdominal surgeries
- Adhesions
- Obesity
- High-risk abdominal conditions
Therefore, many surgeons prefer the Hasson Trocar for complex laparoscopic procedures.
Key Features of Hasson Trocar
Blunt Tip Design
The blunt obturator minimizes tissue trauma and reduces the risk of accidental organ perforation.
Secure Fixation System
The trocar includes suture fixation wings or cones that help secure the cannula firmly in place during surgery.
Gas Leak Prevention
High-quality sealing valves maintain consistent pneumoperitoneum and prevent CO₂ leakage.
Durable Construction
The instrument is commonly manufactured from premium-grade stainless steel and medical-grade materials for long-lasting performance.
Multiple Size Options
Hasson Trocars are available in various diameters such as:
- 5 mm
- 10 mm
- 12 mm
This allows compatibility with different laparoscopic instruments.
Applications of Hasson Trocar
The Hasson Trocar is widely used in several minimally invasive procedures.
General Surgery
- Laparoscopic cholecystectomy
- Hernia repair
- Appendectomy
- Colorectal surgery
Gynecological Surgery
- Hysterectomy
- Ovarian cyst removal
- Endometriosis treatment
Urological Procedures
- Nephrectomy
- Pyeloplasty
- Prostate surgery
Bariatric Surgery
- Gastric bypass
- Sleeve gastrectomy
Because of its controlled entry method, the trocar is highly effective in high-risk surgical cases.
Advantages of Using Hasson Trocar
Enhanced Patient Safety
The open-entry technique significantly lowers the risk of vascular and bowel injury.
Better Surgical Control
Surgeons gain direct visualization during insertion, improving procedural accuracy.
Reduced Complications
The Hasson Trocar helps reduce complications associated with blind trocar insertion.
Excellent Stability
Its fixation mechanism prevents accidental trocar displacement during surgery.
Ideal for Difficult Cases
It is especially useful for patients with adhesions or previous abdominal surgeries.
Difference Between Hasson Trocar and Standard Trocar
| Feature | Hasson Trocar | Standard Trocar |
| Entry Technique | Open Entry | Blind Entry |
| Tip Type | Blunt | Sharp |
| Safety Level | Higher | Moderate |
| Risk of Organ Injury | Lower | Higher |
| Fixation System | Yes | Limited |
| Ideal for Adhesions | Yes | Less Suitable |
Why Surgeons Prefer Hasson Trocar
Surgeons prefer the Hasson Trocar because it provides better control and safer abdominal access. Furthermore, it improves confidence during laparoscopic entry in complex patients.
In addition, many hospitals and surgical centers adopt the Hasson technique as part of their patient safety protocols.
Since minimally invasive surgery continues to grow worldwide, reliable access instruments like the Hasson Trocar remain essential in operating rooms.
Maintenance and Sterilization
Proper cleaning and sterilization are necessary for maintaining surgical performance and patient safety.
Recommended practices include:
- Thorough cleaning after every procedure
- Autoclave sterilization
- Inspection of seals and valves
- Checking blunt obturator alignment
- Safe storage in sterilization trays
Regular maintenance also extends instrument lifespan and ensures optimal surgical efficiency.
Choosing the Right Hasson Trocar
When selecting a Hasson Trocar, healthcare professionals should consider:
- Trocar diameter
- Instrument compatibility
- Quality of sealing system
- Reusable or disposable type
- Ergonomic handling
- Material quality
Choosing a high-quality trocar ensures better surgical outcomes and long-term reliability.
Future of Laparoscopic Access Devices
Laparoscopic technology continues to evolve rapidly. Modern Hasson Trocars now feature:
- Improved ergonomic designs
- Better sealing technology
- Lightweight materials
- Enhanced fixation systems
- Disposable sterile options
As minimally invasive procedures become more advanced, safe access systems will remain critical for surgical success.
Conclusion
The Hasson Trocar plays a vital role in modern laparoscopic surgery by providing secure, controlled, and safe abdominal access. Its blunt-tip design, fixation system, and open-entry technique help reduce complications and improve surgical safety.
Moreover, the trocar is highly valuable in complex and high-risk laparoscopic procedures where patient safety is crucial. Because of its reliability and effectiveness, the Hasson Trocar continues to be a trusted instrument in hospitals and surgical centers worldwide.
For healthcare professionals seeking advanced laparoscopic access solutions, the Hasson Trocar remains an excellent choice for precision and patient protection.
Get Connected:
+91 79909 93062 | +91 63513 72032 | exports@jdmeditech.com