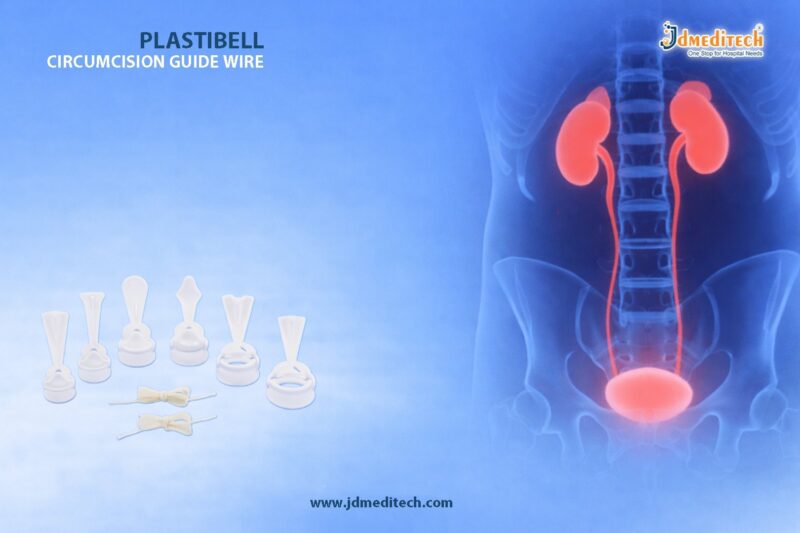
The Plastibell Circumcision Device is a widely used medical tool designed for safe and controlled infant circumcision. Doctors prefer the Plastibell Circumcision Device because it ensures minimal bleeding, reduced complications, and faster healing compared to traditional surgical methods.
In modern pediatric surgery, the Plastibell Circumcision Device has become a trusted solution due to its simplicity, effectiveness, and excellent clinical outcomes.
What is a Plastibell Circumcision Device?
The Plastibell Circumcision Device is a small, sterile plastic ring placed over the glans penis during circumcision. It helps guide the removal of the foreskin while protecting sensitive tissues.
After the procedure, the Plastibell Circumcision Device remains in place for a few days and naturally falls off as the tissue heals.
How the Plastibell Circumcision Device Works
The procedure using the Plastibell Circumcision Device is straightforward and highly controlled:
- The foreskin is gently separated from the glans
- The Plastibell Circumcision Deviceis positioned over the glans
- A surgical thread is tied around the foreskin
- Excess foreskin is removed safely
- The Plastibell Circumcision Devicestays in place until healing begins
This method reduces surgical trauma and ensures precision.
Benefits of Plastibell Circumcision Device
1. Minimal Bleeding
The Plastibell Circumcision Device applies controlled pressure, significantly reducing bleeding during the procedure.
2. Reduced Risk of Infection
Since the Plastibell Circumcision Device protects the surgical site, it lowers infection chances.
3. Faster Healing
Infants recover quickly because the Plastibell Circumcision Device promotes natural healing.
4. No Sutures Required
Unlike traditional methods, the Plastibell Circumcision Device eliminates the need for stitches.
5. Safe and Reliable
The Plastibell Circumcision Device is clinically proven and widely accepted by pediatric surgeons.
Plastibell Circumcision Device in Pediatric Care
The Plastibell Circumcision Device is commonly used for newborns and infants. Pediatricians recommend the Plastibell Circumcision Device due to its predictable outcomes and ease of use.
It is especially beneficial in hospital and clinical settings where safety and efficiency are priorities.
Aftercare Following Plastibell Circumcision Device Procedure
Proper care ensures smooth recovery after using the Plastibell Circumcision Device:
- Keep the area clean and dry
- Avoid unnecessary handling
- Monitor for redness or swelling
- Allow the Plastibell Circumcision Deviceto fall off naturally
Parents should consult a doctor if healing appears delayed.
Possible Risks and Considerations
Although the Plastibell Circumcision Device is safe, some minor risks may include:
- Temporary swelling
- Mild discomfort
- Delayed ring separation
These issues are rare and usually resolve without complications.
Why Choose Plastibell Circumcision Device?
The Plastibell Circumcision Device offers a modern approach to infant circumcision. Its advantages over traditional methods make it a preferred choice for healthcare providers worldwide.
With consistent results and improved patient comfort, the Plastibell Circumcision Device continues to be a leading solution in pediatric surgery.
Conclusion
The Plastibell Circumcision Device is a safe, effective, and widely trusted method for infant circumcision. Its ability to minimize complications, ensure faster healing, and provide reliable results makes it an essential tool in modern medical practice.
Get Connected:
+91 79909 93062 | +91 63513 72032 | exports@jdmeditech.com