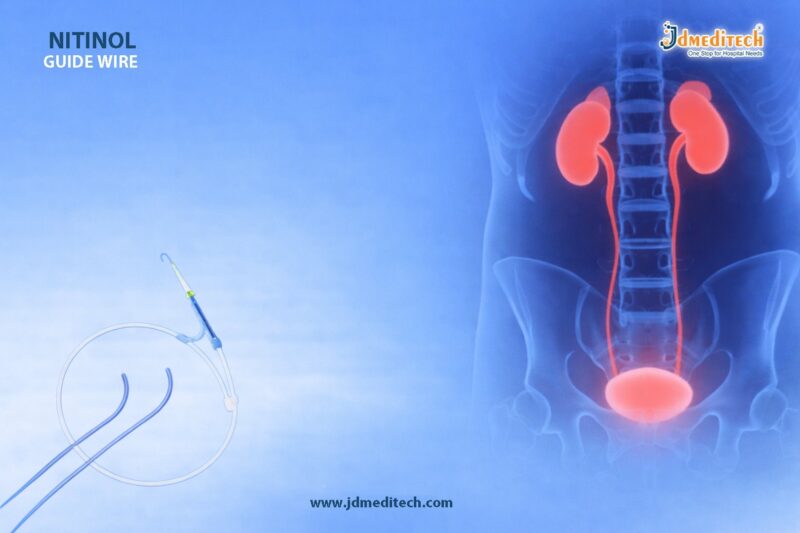
In modern minimally invasive procedures, precision and control are essential. The Nitinol Guide Wire plays a critical role in ensuring smooth navigation through complex anatomical pathways. Thanks to its unique material properties, this advanced medical device combines durability with excellent trackability, making it a preferred choice for urologists and interventional specialists.
Moreover, the growing demand for reliable and flexible guidewires has increased the importance of nitinol-based solutions in today’s healthcare environment.
What is a Nitinol Guide Wire?
A Nitinol Guide Wire is a medical device made from a nickel-titanium alloy known as nitinol. This material is widely recognized for its shape memory and superelasticity, which allow the guidewire to return to its original shape even after bending.
As a result, the Nitinol Guide Wire provides superior maneuverability and consistent performance during complex procedures.
Key Features of Nitinol Guide Wire
1. Exceptional Flexibility and Shape Memory
One of the standout features of the Nitinol Guide Wire is its ability to bend without breaking. It easily adapts to curved anatomical structures while maintaining its original shape.
2. Superior Durability
Unlike traditional guidewires, the Nitinol Guide Wire resists kinking and deformation. Therefore, it ensures long-lasting performance even in demanding clinical environments.
3. Excellent Trackability
The Nitinol Guide Wire is designed for smooth advancement through narrow and tortuous pathways. Consequently, it enhances procedural efficiency and reduces complications.
4. Enhanced Torque Control
Physicians benefit from precise control, as the Nitinol Guide Wire transmits rotational movements effectively from the proximal to distal end.
5. Hydrophilic Coating Compatibility
Many variants of the Nitinol Guide Wire come with hydrophilic coatings. This feature reduces friction and ensures effortless navigation.
Applications of Nitinol Guide Wire
The Nitinol Guide Wire is widely used across multiple medical specialties due to its versatility.
Urology
It is commonly used in procedures such as:
- Ureteroscopy
- Stone management
- Catheter placement
Cardiology
In cardiovascular interventions, the Nitinol Guide Wire assists in navigating blood vessels during angioplasty and stent placement.
Gastroenterology
It is also utilized in endoscopic procedures for accessing bile ducts and other gastrointestinal pathways.
Advantages Over Conventional Guidewires
Compared to stainless steel guidewires, the Nitinol Guide Wire offers several advantages:
- Greater flexibility without permanent deformation
- Improved patient safety due to reduced trauma
- Better navigation in complex anatomy
- Longer lifespan and reliability
Because of these benefits, healthcare professionals increasingly prefer the Nitinol Guide Wire for advanced procedures.
How to Choose the Right Nitinol Guide Wire
Selecting the appropriate Nitinol Guide Wire depends on several factors:
- Procedure type – Urological, cardiac, or GI
- Wire diameter and length
- Coating type – Hydrophilic or PTFE
- Tip configuration – Straight or J-tip
Therefore, understanding clinical requirements helps in choosing the most suitable guide wire.
Safety and Handling Considerations
Although the Nitinol Guide Wire is highly durable, proper handling is essential:
- Avoid excessive force during insertion
- Maintain sterility at all times
- Inspect the wire before use
- Follow manufacturer guidelines
These precautions ensure optimal performance and patient safety.
Future of Nitinol Guide Wire Technology
With ongoing advancements in medical technology, the Nitinol Guide Wire continues to evolve. Innovations such as improved coatings, enhanced tip designs, and hybrid materials are further enhancing its performance.
As a result, the Nitinol Guide Wire is expected to remain a cornerstone of minimally invasive procedures.
Conclusion
The Nitinol Guide Wire represents a perfect combination of durability, flexibility, and excellent trackability. Its advanced design supports safe and efficient navigation across various medical specialties.
For healthcare professionals seeking precision and reliability, the Nitinol Guide Wire is undoubtedly an essential tool in modern clinical practice.
Get Connected:
+91 79909 93062 | +91 63513 72032 | exports@jdmeditech.com