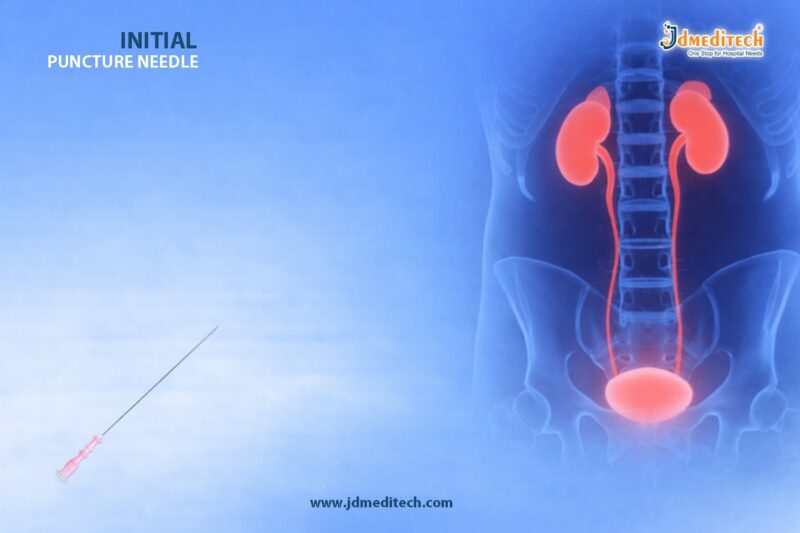
The initial puncture needle is a critical medical instrument used to establish safe and accurate percutaneous access during various diagnostic and therapeutic procedures. It plays a vital role in interventional radiology, urology, and minimally invasive surgeries. Because precision is essential in these procedures, the initial puncture needle helps clinicians access targeted anatomical structures with minimal trauma. As a result, it significantly improves patient safety and procedural success rates.
What is an Initial Puncture Needle?
The initial puncture needle is a specially designed sharp needle used to create the first entry point into the body through the skin. Typically, it is used in procedures such as PCNL (Percutaneous Nephrolithotomy), biopsy, drainage, and vascular access. Moreover, it allows accurate placement under imaging guidance like ultrasound or fluoroscopy.
Key Characteristics
- Sharp beveled tip for precise penetration
- High-quality stainless steel construction
- Echogenic markings for better visibility
- Ergonomic hub for improved grip and control
- Available in various lengths and gauges
Applications of Initial Puncture Needle
The initial puncture needle is widely used across multiple medical specialties. Therefore, its versatility makes it an indispensable tool in modern healthcare.
Common Uses
- Percutaneous nephrolithotomy (PCNL) procedures
- Renal access and stone removal
- Tissue biopsy procedures
- Fluid aspiration and drainage
- Vascular access interventions
Because of its precision, the initial puncture needle ensures minimal tissue damage while achieving accurate entry.
Benefits of Using Initial Puncture Needle
The use of an initial puncture needle offers several advantages, especially in minimally invasive procedures. In addition, it enhances both procedural efficiency and patient outcomes.
Major Benefits
- High accuracy during percutaneous access
- Reduced risk of complications
- Minimal tissue trauma
- Enhanced control for clinicians
- Compatibility with imaging guidance systems
Furthermore, the initial puncture needle supports faster recovery due to reduced invasiveness.
Design and Material Quality
The design of the initial puncture needle focuses on safety, precision, and durability. For instance, it is manufactured using medical-grade stainless steel to ensure strength and corrosion resistance. Additionally, echogenic tips improve visibility under ultrasound, which allows accurate targeting.
Advanced Features
- Anti-corrosive and biocompatible material
- Smooth surface for easy insertion
- Optimal flexibility with strength
- Secure hub connection for stability
As a result, the initial puncture needle delivers consistent performance across procedures.
Role in Safe Percutaneous Access
Safe percutaneous access is the foundation of many minimally invasive procedures. Therefore, the initial puncture needle plays a crucial role in ensuring correct entry into the targeted area. With imaging guidance, clinicians can avoid critical structures and reduce complications.
Moreover, the initial puncture needle enables controlled penetration, which improves overall procedural safety. Consequently, it is considered an essential instrument in interventional medicine.
How to Choose the Right Initial Puncture Needle
Selecting the appropriate initial puncture needle depends on the procedure type and patient requirements. Thus, healthcare professionals should consider several factors before use.
Selection Factors
- Needle gauge and length
- Type of procedure
- Imaging compatibility
- Required flexibility and rigidity
- Manufacturer quality standards
Choosing the correct initial puncture needle ensures optimal results and reduces procedural risks.
Why Choose JDMeditech Initial Puncture Needle
At www.jdmeditech.com, we provide high-quality initial puncture needle solutions designed to meet international medical standards. Our products are trusted by healthcare professionals for their reliability and performance.
Our Advantages
- Precision-engineered products
- Strict quality control standards
- Wide range of medical instruments
- Competitive pricing
- Trusted supplier and manufacturer
Because of our commitment to quality, JDMeditech remains a preferred choice in the medical industry.
Conclusion
The initial puncture needle is an essential tool for safe percutaneous access in modern medical procedures. It ensures precision, safety, and efficiency while minimizing complications. As minimally invasive techniques continue to grow, the importance of the initial puncture needle becomes even more significant. Therefore, choosing a high-quality product from a trusted provider like JDMeditech ensures optimal clinical outcomes.
Get Connected:
+91 79909 93062 | +91 63513 72032 | exports@jdmeditech.com