Bipolar TURP: Safe and Advanced Treatment for Enlarged Prostate
What Is Bipolar TURP?
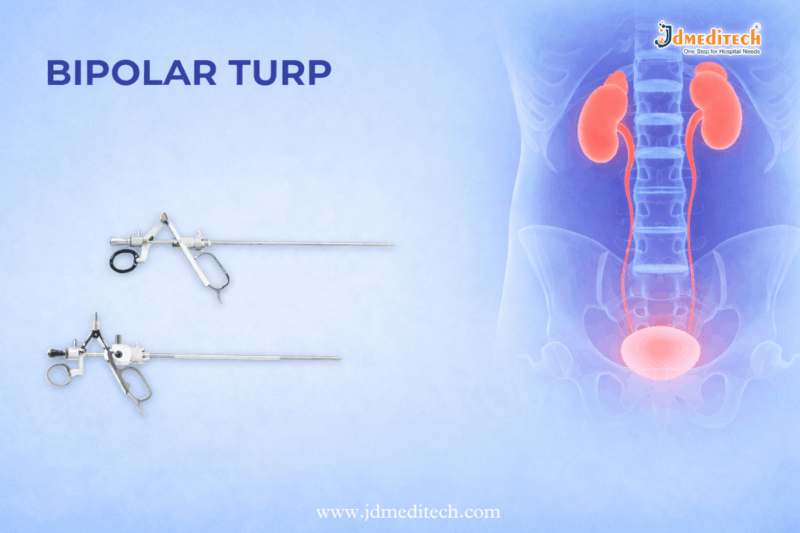
Bipolar TURP is a modern surgical procedure used to treat an enlarged prostate. Doctors often recommend Bipolar TURP for men with moderate to severe urinary symptoms caused by benign prostatic hyperplasia (BPH). This procedure removes extra prostate tissue and helps improve urine flow.
Unlike older methods, Bipolar TURP uses bipolar energy with saline irrigation. As a result, it offers better safety and improved surgical control. Because of these benefits, many hospitals and urology specialists now prefer Bipolar TURP.
Why Is Bipolar TURP Needed?
An enlarged prostate can press against the urethra and block the normal flow of urine. Therefore, patients may face several uncomfortable symptoms. In many cases, Bipolar TURP is advised when medicines no longer provide enough relief.
Common symptoms include:
- Frequent urination
- Difficulty starting urination
- Weak urine stream
- Night-time urination
- Incomplete bladder emptying
- Sudden urge to urinate
- Urinary retention
When these symptoms become severe, Bipolar TURP can provide long-term relief.
How Bipolar TURP Works
During Bipolar TURP, the surgeon inserts a resectoscope through the urethra. No external cut is needed. Then the surgeon uses bipolar electrical energy to remove the extra prostate tissue blocking the urinary passage.
At the same time, saline solution is used for irrigation. This improves visibility and also lowers the risk of complications linked with non-saline fluids. After tissue removal, the surgeon places a catheter for temporary drainage.
In most cases, Bipolar TURP is completed within 60 to 90 minutes.
Key Benefits of Bipolar TURP
There are many reasons why Bipolar TURP is considered a preferred option for BPH treatment.
1. Better Safety
Bipolar TURP uses saline solution, which reduces the risk of TUR syndrome. This makes the procedure safer than traditional monopolar methods.
2. Less Bleeding
Because bipolar energy offers better coagulation, Bipolar TURP helps control bleeding during surgery.
3. Faster Recovery
Most patients recover faster after Bipolar TURP. In addition, hospital stay is often shorter.
4. Improved Precision
The system allows accurate cutting and effective removal of obstructing tissue.
5. Suitable for Many Patients
Doctors may choose Bipolar TURP for elderly patients or for those who need a safer surgical option.
Bipolar TURP vs Monopolar TURP
Both procedures treat enlarged prostate, but Bipolar TURP offers several important advantages.
| Feature | Bipolar TURP | Monopolar TURP |
| Energy system | Bipolar | Monopolar |
| Irrigation fluid | Saline | Non-saline fluid |
| TUR syndrome risk | Very low | Higher |
| Bleeding control | Better | Moderate |
| Recovery time | Faster | Slower |
| Safety profile | Higher | Lower |
Because of these differences, many surgeons now prefer Bipolar TURP over monopolar TURP.
Who Can Benefit From Bipolar TURP?
Bipolar TURP is usually recommended for men who:
- Have moderate to severe BPH symptoms
- Do not respond well to medication
- Experience repeated urinary retention
- Need effective prostate tissue removal
- Want a minimally invasive treatment option
However, the final decision depends on the patient’s condition, prostate size, and overall health.
Recovery After Bipolar TURP
Recovery after Bipolar TURP is generally smooth. Most patients stay in the hospital for a short period. The catheter is usually removed within one to two days.
After surgery, patients may notice:
- Mild discomfort during urination
- Small amounts of blood in urine
- Frequent urge to urinate for a few days
These symptoms usually improve with time. Still, proper care is important after Bipolar TURP.
Recovery Tips
- Drink enough water
- Avoid heavy lifting
- Follow medical advice carefully
- Take prescribed medicines on time
- Attend all follow-up visits
In most cases, patients return to normal daily activities within two to three weeks after Bipolar TURP.
Possible Risks of Bipolar TURP
Although Bipolar TURP is considered safe, every surgery carries some risk. Possible complications may include:
- Urinary tract infection
- Mild bleeding
- Temporary difficulty in urination
- Retrograde ejaculation
- Temporary urinary incontinence
However, serious complications are uncommon, especially when Bipolar TURP is performed by experienced surgeons.
Why Bipolar TURP Is a Preferred Choice
Today, Bipolar TURP is widely used because it combines safety, efficiency, and reliable results. It offers better control during surgery and supports quicker recovery. Moreover, it reduces the risk of some complications seen in older TURP methods.
For these reasons, Bipolar TURP has become a trusted solution for the treatment of enlarged prostate.
Conclusion
Bipolar TURP is a safe, advanced, and effective treatment for men suffering from enlarged prostate symptoms. It improves urine flow, reduces discomfort, and supports faster recovery. In addition, it offers clear benefits over traditional monopolar techniques.
If you are looking for an advanced BPH treatment option, Bipolar TURP may be the right choice. Always consult a qualified urology specialist for proper diagnosis and treatment planning.
Get Connected:
+91 79909 93062 | +91 63513 72032 | exports@jdmeditech.com