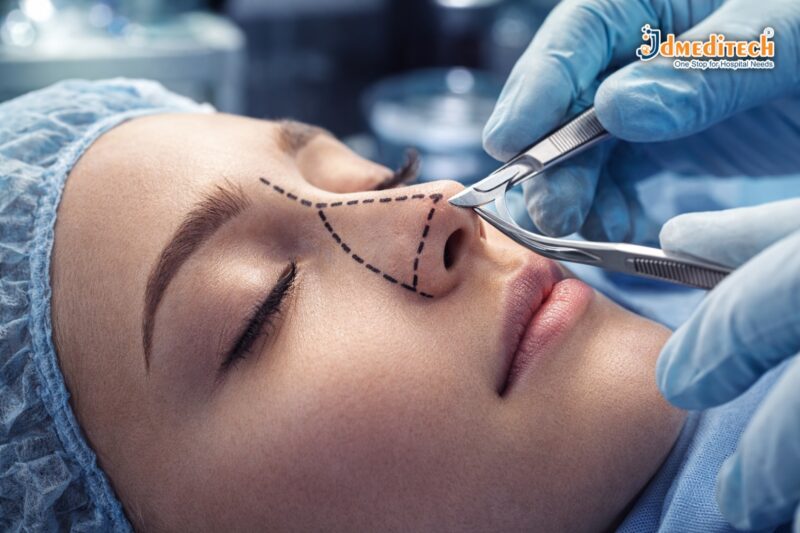
Rhinoplasty is a surgical procedure designed to change the shape, size, or structure of the nose. It can be performed for cosmetic reasons or to correct medical problems such as a deviated septum.
Types of Rhinoplasty
- Cosmetic Rhinoplasty – Improves the appearance of the nose
- Functional Rhinoplasty – Corrects breathing problems
- Revision Rhinoplasty – Fixes previous nose surgery issues
- Non-Surgical Rhinoplasty – Uses fillers for temporary changes
Rhinoplasty Procedure
Rhinoplasty surgery is typically performed under general or local anesthesia and takes about 1 to 3 hours.
Step-by-Step Procedure
- Administration of anesthesia
- Incision (open or closed technique)
- Reshaping the nasal bones and cartilage
- Correction of septum if required
- Closing the incision and applying a splint
Benefits of Rhinoplasty Surgery
- Improves facial balance and symmetry
- Enhances self-confidence
- Corrects breathing issues
- Repairs nasal injuries
- Provides permanent results
Risks and Complications
Like any surgical procedure, rhinoplasty carries some risks:
- Infection
- Bleeding
- Swelling and bruising
- Breathing difficulties
- Unsatisfactory results (rare)
Rhinoplasty Recovery Time
Recovery varies from person to person but generally follows this timeline:
- 1 Week – Splint removal
- 2 Weeks – Bruising reduces
- 1 Month – Visible improvement
- 3–6 Months – Healing progresses
- 1 Year – Final results
Recovery Tips
- Avoid strenuous activities
- Keep head elevated while sleeping
- Follow surgeon’s instructions
- Avoid wearing glasses initially
Who is a Good Candidate?
You may be a good candidate for rhinoplasty if:
- You are physically healthy
- You have realistic expectations
- Your facial growth is complete
- You want to improve nose appearance or function
Conclusion
Rhinoplasty surgery is a safe and effective procedure for enhancing both the appearance and function of the nose. With proper consultation and care, patients can achieve natural-looking and satisfying results. Always consult a qualified plastic surgeon to determine the best approach for your needs.
Get Connected:
+91 79909 93062 | +91 63513 72032 | exports@jdmeditech.com